TL;DR
- The Study: A Nature Medicine study of 18,701 participants across 34 countries (April 2026) finds that combined physical and social environmental exposures accelerate brain aging up to 9.1 times more than a clinical dementia diagnosis alone.
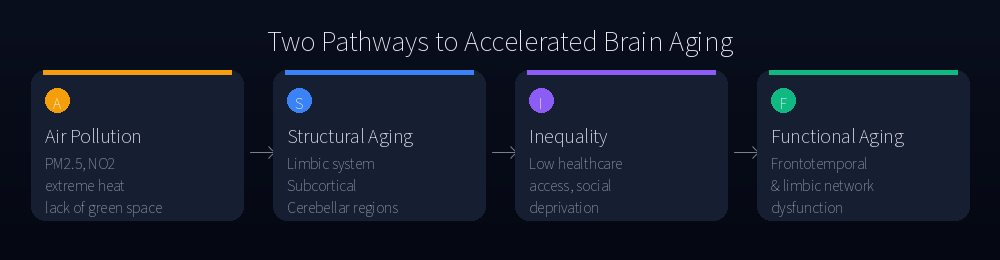
- The Nuance: Air pollution targets the brain’s memory and emotion centers (structural aging); inequality and poor healthcare access target its decision-making and social networks (functional aging) — two distinct pathways.
- The Action: Three evidence-backed steps you can take now, and what requires structural change.
Where You Live May Be Aging Your Brain Faster Than a Dementia Diagnosis
Here is an uncomfortable question: What if the city you live in, the air you breathe, and the healthcare system you belong to are doing more damage to your brain than a mild cognitive impairment diagnosis?
According to a landmark study published April 3, 2026 in Nature Medicine, the answer may be yes — and the effect can be up to 9.1 times stronger.
The research, led by Agustina Legaz and Sebastian Moguilner — Atlantic Fellows at the Global Brain Health Institute, affiliated with institutions including Harvard University, the University of Edinburgh, and the Latin American Brain Health Institute (BrainLat) — analyzed data from 18,701 participants across 34 countries, including healthy adults and people living with Alzheimer’s disease, frontotemporal lobar degeneration, and mild cognitive impairment.
This is not a study about one bad day of smog. It is about the cumulative, compounding weight of the environment on the brain over a lifetime.
The Exposome: Why Single-Factor Studies Miss the Point
For decades, researchers have studied environmental risk factors in isolation. Air pollution is bad for the brain. Economic inequality degrades cognitive health. Lack of green space increases stress. Each of these findings is real, but they tell only a fragment of the story.
This study introduced a different lens: the exposome — the total accumulation of every environmental and social exposure a person encounters from birth. The researchers simultaneously analyzed 73 country-level factors spanning air pollution, climate variability, green space availability, water quality, socioeconomic inequality, healthcare infrastructure, and political stability indicators.
The result was unambiguous. Aggregated exposome models explained 15.5 times more variance in brain aging than any single exposure factor (delta AIC: 2,034–3,127). Looking at just one variable — say, PM2.5 levels — means seeing roughly 6.5% of the picture.
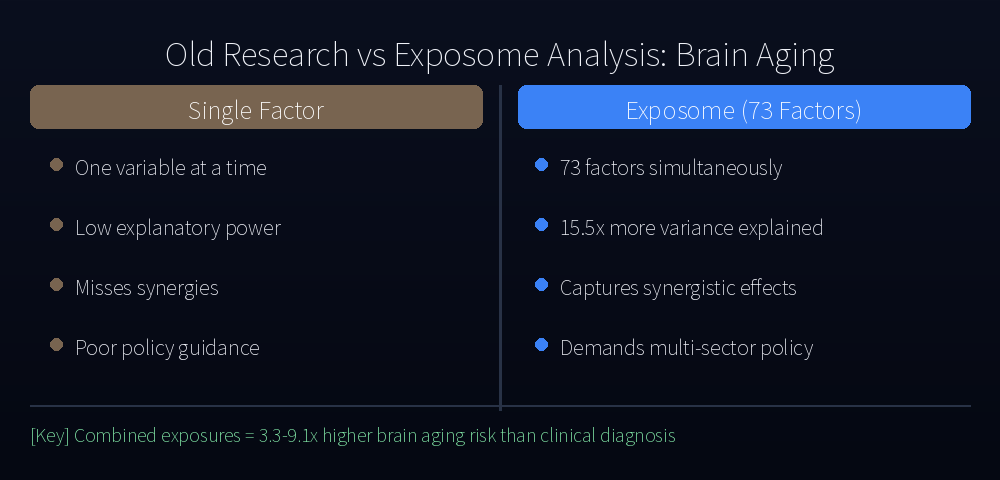

The implication is profound: policies addressing only one environmental factor at a time are structurally insufficient.
Two Pathways, Two Different Damages
One of the study’s most clinically significant findings is that physical and social exposures damage the brain in distinct, measurable ways.
Physical exposures — primarily air pollution, extreme heat events, and lack of green space — are associated with accelerated structural brain aging. The regions most affected are the limbic system, subcortical structures, and the cerebellum: areas responsible for memory formation, emotional regulation, and autonomic functions. Think of this as the hardware degrading.
Social exposures — inequality, inadequate healthcare access, and the absence of social protection networks — are associated with accelerated functional brain aging. The regions most affected are frontotemporal and limbic networks: areas responsible for complex decision-making, social behavior, and language processing. Think of this as the software losing coherence.
When both pathways operate simultaneously — when someone lives in a polluted environment and a high-inequality society with limited healthcare access — the risk of accelerated brain aging rises to 3.3–9.1 times that seen with clinical diagnoses of MCI or dementia alone.
To be clear: this does not mean pollution and inequality “cause” dementia. The relationship is more nuanced. What it means is that the environmental context in which a person ages can amplify or attenuate neurological vulnerability to a degree that rivals, and sometimes exceeds, the impact of established clinical diagnoses.
The Protective Side of the Equation
The study did not only identify risks. It also confirmed protective factors that can slow biological brain aging:
- Socioeconomic equality: Countries with lower Gini coefficients (more equal income distribution) showed slower functional brain aging across populations.
- Access to universal healthcare: Strong healthcare infrastructure was consistently associated with reduced brain aging risk in the social exposome pathway.
- Green space availability: Adequate urban green space (parks, forests, green corridors) emerged as a measurable buffer against the structural brain aging driven by physical exposures.
These findings are not merely statistical. They suggest that investments in urban green infrastructure, healthcare equity, and income redistribution have quantifiable neurological returns.
What This Means For You
The researchers are explicit that this is not a problem individuals can solve alone. The exposome is, by definition, a societal and structural phenomenon. Nevertheless, current evidence supports several individual-level actions.
1. Protect your physical exposome — today:
- On high-pollution days (PM2.5 > 35 μg/m³), wear a well-fitted N95 or equivalent respirator when outdoors. These reduce PM2.5 inhalation by over 95%.
- Use HEPA air purifiers indoors, particularly in bedrooms where you spend 7–8 hours daily. Indoor PM2.5 can be as damaging as outdoor levels in poorly ventilated spaces.
- Prioritize green space exposure. A Stanford University study (2015, PNAS) found that 90 minutes of nature walking reduced neural activity in regions associated with repetitive negative thinking — the same regions implicated in this study’s structural aging pathway.
2. Protect your social exposome — invest in connection:
- Social isolation is both a symptom and a driver of the social exposome risk. Regular, in-person social engagement is associated with preserved frontotemporal network function, the exact region most vulnerable to social exposome damage.
- If you are a caregiver, advocate, or clinician: environments that reduce social isolation in older adults may be functioning, in part, as neurological interventions.
3. Know your environment’s profile:
- Understanding the specific exposome risks in your city — local PM2.5 averages, healthcare access indices, urban green coverage — provides actionable context. National environmental health agencies publish this data; the WHO Global Air Quality Database is a starting point.
What requires structural change (not personal habit):
- Enforcement of WHO PM2.5 guidelines (5 μg/m³ annual mean) — currently exceeded by most major cities worldwide.
- Urban planning mandates for minimum green space per capita in new developments.
- Healthcare access equity, particularly in low- and middle-income countries where the social exposome burden is highest.
Study Limitations to Keep in Mind
Responsible reporting on health research requires acknowledging what this study cannot tell us:
- Country-level indicators: The exposome factors were measured at the national level. Within-country variation — between cities, neighborhoods, or individuals — can be substantial, and this study does not capture it.
- Correlation, not proven causation: This is a large-scale observational study. While the associations are robust and the sample size is exceptional, establishing that environmental exposures cause accelerated brain aging requires longitudinal intervention studies that are still ongoing.
- Mixed participant pool: The study included both healthy participants and those with neurodegenerative diagnoses. Findings should be interpreted with nuance when extrapolating to healthy populations exclusively.
The authors acknowledge these limitations directly in the paper. A companion News and Views editorial in the same issue of Nature Medicine (“Exposure to negative physical and social factors accelerates brain aging,” April 2026) validates the study’s methodological approach while calling for follow-up research.
The Bottom Line
Brain aging has long been framed as a private, biological inevitability — written into DNA, measurable in plaques and tangles. This study reframes it as, in significant part, a public health outcome shaped by the environment we collectively build and tolerate.
The city you live in. The air your children breathe on the way to school. The distance to the nearest park. The quality of the healthcare system available to your parents as they age. Each of these, compounded across a lifetime, adds up to something measurable in the structure and function of the brain itself.
That is a different kind of finding. And it demands a different kind of response.

This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Source: Legaz A, Moguilner S, Hernandez H, Ibanez A, et al. “The exposome of brain aging across 34 countries.” Nature Medicine, April 3, 2026. DOI: 10.1038/s41591-026-04302-z