TL;DR
- The Study: Nature Medicine (April 2026), 18,701 participants, 34 countries — 73 physical and social environmental factors analyzed against brain age.
- The Key Finding: Combined environmental exposure (exposome) explained up to 15.5× more variance in brain aging than any single factor — with an effect size comparable to mild cognitive impairment and dementia.
- The Implication: Brain health is not just about personal choices. The neighborhood you live in, the air you breathe, and the social conditions you were born into may be silently aging your brain.
A Study That Reframes the Dementia Conversation
For decades, public health messaging around dementia and brain aging has followed a familiar script: exercise more, eat better, sleep enough, stay mentally active. All of that advice is evidence-based. But a new study published in Nature Medicine in April 2026 adds something the script has been missing — the place itself.
The research team analyzed brain imaging data from 18,701 participants across 34 countries — a cohort spanning healthy individuals alongside those diagnosed with Alzheimer’s disease, frontotemporal lobar degeneration, and mild cognitive impairment (MCI). Against this data, they mapped 73 country-level environmental and social variables, a framework they term the exposome: the sum total of all non-genetic exposures across a lifetime.
The results were stark. When the full exposome was modeled together, it explained up to 15.5 times more variation in brain age than any single environmental factor could on its own. The combined effect of environmental, social, and political conditions on brain aging was comparable in magnitude to what MCI and dementia do to the brain — conditions we classify as clinical diseases.
Two Pathways to an Older Brain
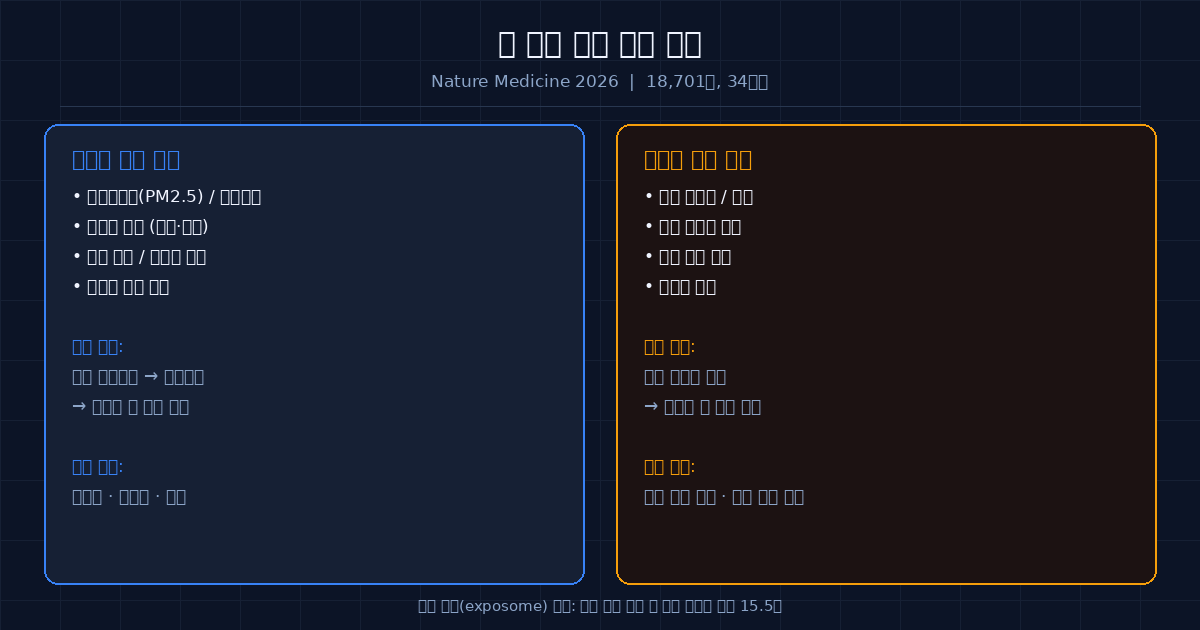
The study’s architecture reveals a nuanced two-track mechanism.
Physical exposome — encompassing air pollution (particularly PM2.5), extreme temperatures, noise, UV exposure, green space access, and housing quality — was primarily associated with structural brain aging. Affected regions included the limbic system, subcortical structures, and cerebellum: areas central to emotional processing, memory consolidation, and motor coordination. The proposed pathway runs through oxidative stress and neuroinflammation. Fine particulate matter (PM2.5) can cross the blood-brain barrier and reach neural tissue directly via the olfactory nerve, triggering chronic immune responses that slowly erode brain tissue.
Social exposome — capturing income inequality, healthcare access, educational attainment, and social isolation — was more strongly associated with functional brain aging: the kind that shows up as declining cognitive performance before structural changes become visible on a scan. The mechanism here runs through cognitive reserve — the brain’s adaptive capacity built up through education, social engagement, and mental stimulation. When social conditions deny people these inputs, the brain builds less reserve and ages faster under stress.
Both pathways were validated cross-sectionally and longitudinally, remaining significant after adjusting for age, sex, race/ethnicity, scanner type, and data quality. The effects persisted across clinical subgroups and were consistent across the full geographic span of the study.
The Numbers Behind the Claim

The 15.5× multiplier for the combined exposome model is not the only striking number in this research. Several converging data points strengthen the picture:
- A meta-analysis in Lancet Planetary Health (2025) found that long-term PM2.5 exposure is associated with at least a 14% increase in dementia risk across the pooled population.
- Nature Aging (2025) confirmed a significant association specifically between PM2.5 and Alzheimer’s disease — not just general cognitive decline.
- A large retrospective cohort study using South Korea’s National Health Insurance database (5.2 million older adults, 2010–2019) found that higher concentrations of PM10, PM2.5, and NO2 significantly predicted incident dementia — one of the most robust national-level confirmations of this link anywhere in the world.
The body of evidence is now substantial enough that researchers are no longer asking whether air pollution affects the brain. The question has shifted to how much, through which pathways, and what to do about it.
What This Means For You
The practical implications split across two levels: what individuals can do today, and what structural change this research demands.
Individual-level actions:
-
Manage indoor air quality. Most people spend over 90% of their time indoors, but indoor PM2.5 concentrations typically run at 30–60% of outdoor levels — and can spike much higher when outdoor air is poor or when cooking with gas. A HEPA-filter air purifier in your sleeping and living spaces is among the most evidence-supported investments for reducing daily neurological exposure.
-
Time outdoor exercise around air quality. Exercise is strongly protective for brain health — but vigorous outdoor activity on high-pollution days substantially increases the volume of PM2.5 inhaled. On days when air quality is poor (check your local AQI app), move workouts indoors or shift them to early morning hours when pollution tends to be lower.
-
Prioritize social connection deliberately. Social isolation emerged as an independent risk factor for functional brain aging in this study. Maintaining regular, meaningful contact with others — not just passive digital consumption — is associated with slower cognitive decline. This doesn’t require grand social events: a regular phone call with a close friend, joining a local class, or volunteering provides meaningful cognitive reserve.
-
Protect your sleep. Inadequate sleep impairs the brain’s glymphatic system — the overnight waste-clearance mechanism that flushes neurotoxic proteins (including amyloid-beta, implicated in Alzheimer’s). The evidence base for 7–9 hours of sleep as a brain-protective behavior is now very strong.
What individuals cannot do:
It would be misleading to end here. The study’s authors are explicit: their findings “underscore the need for multisectoral and structural policy responses to address physical, social, and political inequities.” A HEPA filter does not fix an urban air quality crisis. Access to healthcare advice is not equally available across income levels. The exposome, by its definition, is shaped largely by forces outside any one person’s control.
Study Limitations Worth Knowing
This research is large, rigorous, and multinationally validated — but transparency demands noting its constraints.
The study is primarily cross-sectional in design, which limits its ability to establish definitive causal direction (though longitudinal components were included and showed consistent results). Individual genetic sensitivity to environmental exposures — which varies substantially — was not fully controlled. Country-level environmental variables are aggregate measures that may not capture local variation within nations. And the study population, while broad, may not represent all socioeconomic strata equally.
These caveats do not undermine the findings, but they should shape how firmly readers translate correlations into personal health decisions. The effect sizes are real and meaningful; the precise dose-response relationships for any given individual remain uncertain.
The Bottom Line
The Nature Medicine study of April 2026 is not a counsel of despair. It is a recalibration: brain health is shaped by choices, yes — but also by the ambient conditions of the world you inhabit.
The finding that 73 environmental factors, working together, can age the brain at the rate of a clinical neurodegenerative condition is both alarming and, paradoxically, cause for optimism. If environments can accelerate brain aging, they can also be changed to slow it. That requires both individual action and collective will.
For now: check your air quality, protect your sleep, maintain your social connections — and stay informed as the science continues to develop.
This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
References:
- Xia et al. (2026). “The exposome of brain aging across 34 countries.” Nature Medicine. doi: 10.1038/s41591-026-04302-z
- Tsai et al. (2025). “Long-term air pollution exposure and incident dementia: a systematic review and meta-analysis.” Lancet Planetary Health.
- Steele et al. (2025). “A systematic review with a Burden of Proof meta-analysis of health effects of long-term ambient PM2.5 exposure on dementia.” Nature Aging.
- Kim et al. (2025). “Long-term exposure to air pollution and incident Alzheimer’s disease among older adults in Korea.” Environmental Science and Pollution Research.
- Chung et al. (2024). “Ambient PM2.5 exposure and rapid population aging: A double threat to public health in the Republic of Korea.” Science of the Total Environment.